Current Projects
Prediction of Motor Responses in Transcranial Magnetic Stimulation with Deep Neural Network using Neuroanatomy and Functional Connectivity
Funding: VCU Breakthroughs Fund
Collaboration: Dr. Peterson and VCU students, Dr. Ravi Hadimani and Biomagnetics Lab, Dr. Jayasimha Atulasimha, Dr. Liangsuo Ma
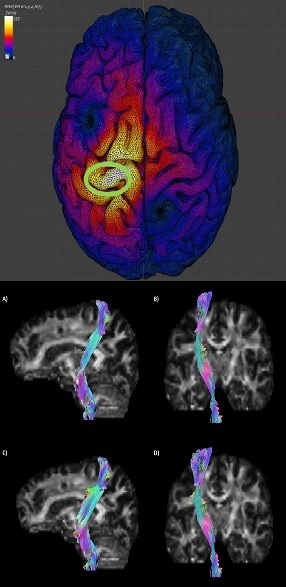
Project Summary: Transcranial magnetic stimulation (TMS) parameters used for treatment or diagnosis depend on the neuroanatomy and functional connectivity of the subjects. We are developing Deep Convolutional Neural Networks capable of predicting TMS induced motor evoked potential based on the neuroanatomy and functional connectivity of the targeted motor network in the brain. This work will lead to better clinical treatment using TMS by informing proper dosing and patient selection.

Home-Based Immersive Virtual Reality and Spinal Stimulation for Upper Limb Rehabilitation in Tetraplegia
Funding: Dept. of Defense Congressionally Directed Medical Research Programs, Spinal Cord Injury Research Program
Collaboration: Dr. Peterson and VCU students, Immersive Experience Labs, Zina Trost, and Ashraf Gorgey.
Project Summary: The objective of our study is to develop a home-based training platform and instructions for Service Members, Veterans, and civilians with spinal cord injury (SCI)-related tetraplegia to improve their ability to use their arms and hands. The platform we are developing with lived-experience stakeholders consists of electrical stimulation applied to the back of the neck while users participate in virtual reality arm and hand training.


Quantification of Shoulder Pathology and Manual Wheelchair Propulsion in Children and Adults with Spinal Cord Injury using Advanced Biomechanical Modeling and Diagnostic Imaging
Funding: Eunice Kennedy Shriver National Institute of Child Health & Human Development
Collaboration: This research is led by Dr. Brooke Slavens (University of Wisconsin- Milwaukee), in collaboration with VCU’s REALab, and researchers and clinicians at Northwestern University, Shriners Hospitals for Children – Chicago, Froedtert and the Medical College of Wisconsin, and the Clement J. Zablocki VA Medical Center.
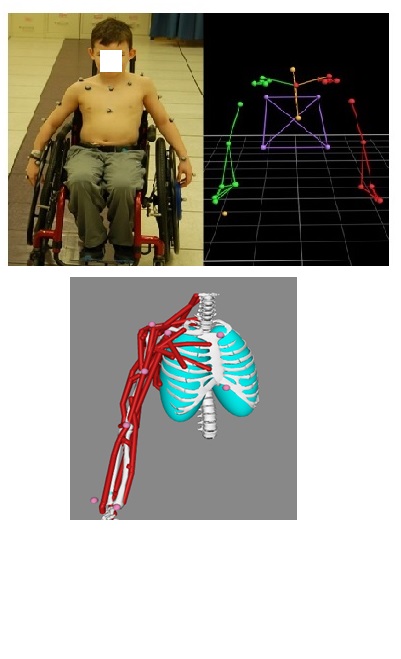
Project Summary: The wheelchair is one of the most widely used assistive mobility devices impacting more than 3.6 million people in the U.S. over the age of 15, 90% of whom use manual wheelchairs. Spinal cord injury (SCI) is a leading cause for wheelchair use. Wheelchair use has detrimental consequences to the health of the user, including shoulder pain and pathology. These complications significantly affect manual wheelchair users throughout their lifespan by reducing quality of life. To improve the quality of life of wheelchair users, there is a need for the prevention of shoulder pain and pathology in manual wheelchair users. This project aims to elucidate the contributing mechanisms of shoulder dysfunction in patients with pediatric-onset SCI and adult-onset SCI through knowledge of joint dynamics, pain, and pathology transitionally across children and adults.

Virginia Consortium for Spinal Cord Injury Care
Funding: National Institute on Disability, Independent Living and Rehabilitation Research Spinal Cord Injury Model Systems
Project Summary: The goal of this center is to enhance upper extremity function in persons with tetraplegia and to improve the equitable delivery, quality, and coordination of interdisciplinary spinal cord injury (SCI) rehabilitation across the healthcare continuum. Project objectives include: (1) evaluating the efficacy of home-based, blood flow restriction-enhanced, neuromuscular, electrical stimulation with or without trans-spinal stimulation on upper extremity function in people with tetraplegia; (2) enrolling and following a diverse group of people with traumatic SCI in the National SCIMS database; (3) leading module research to accelerate equitable care and outcomes for people from racial and ethnic minority groups with traumatic SCI; and (4) translating site specific and collaborative research findings into usable, accessible, and inclusive products for clinicians, consumers, and the general public.
Recent Completed Projects
Intermittent Theta Burst Stimulation to Promote Motor Re-education
Funding: National Center of Neuromodulation for Rehabilitation
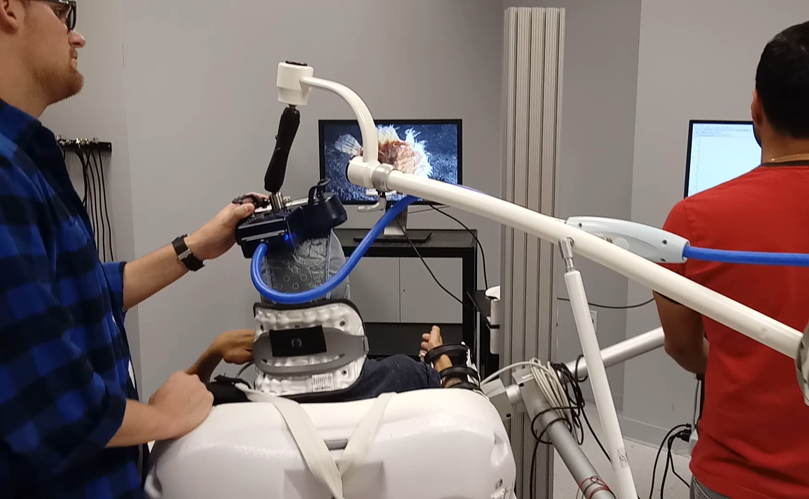
Project Summary: A repetitive, non-invasive brain stimulation technique referred to as theta burst stimulation can modulate corticomotor excitability and therefore has great rehabilitative potential for individuals with neurologic deficits, including individuals with spinal cord injury (SCI). In particular, intermittent theta burst stimulation (iTBS) can increase corticomotor excitability and may be a useful adjunct to physical rehabilitation to promote motor re-education after upper limb reconstruction in individuals with tetraplegia. The long-term goal of our research is to determine whether iTBS combined with physical rehabilitation can improve motor re-education. As a first step, the purpose of this study was to determine the effect of iTBS on corticomotor excitability of proximal muscles in nonimpaired individuals and individuals with tetraplegia.
Development of Clinical Measures to Guide Neuromodulation Therapies
Funding: Virginia Commonwealth University Center for Clinical and Translational Research Endowment Fund (UL1TR000058 from the National Center for Advancing Translational Sciences)
Project Summary: Activation of upper limb muscles is important for independent living after cervical spinal cord injury (SCI) that results in tetraplegia. Individuals with tetraplegia rely on the upper limbs to perform daily self-care activities. Unfortunately, upper limb pain and injury resulting from muscle weakness are significant problems in tetraplegia that result in further debilitation and loss of independence. An emerging approach to address post-SCI muscle weakness is modulation of the nervous system via non-invasive electrical stimulation to re-supply nerve to paralyzed muscle fibers. To direct neuromodulation as an adjunct to physical rehabilitation, clinicians need more informative measures that can indicate changes in the nerve supply to muscle. The purpose of this project is to develop innovative methodology to reliably assess changes in nerve supply to muscle and indicate the location of the nervous system that is performing suboptimal. Neuromodulation techniques can then be targeted to precise locations of the nervous system.